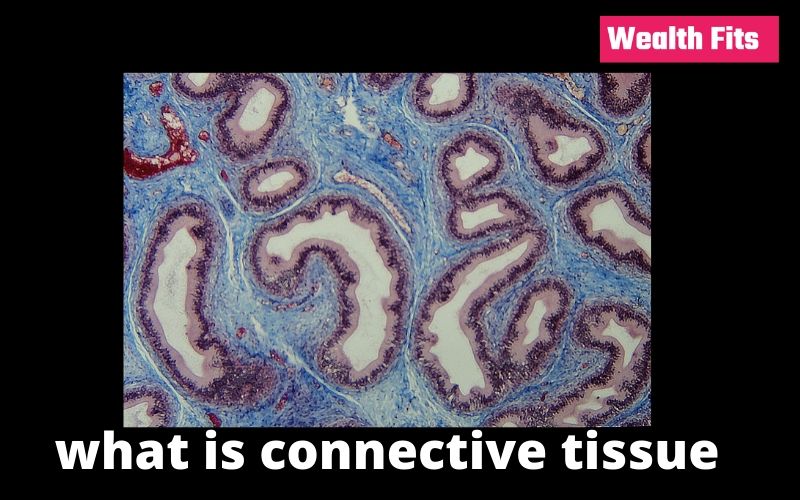
The connective tissue has the function of supporting, joining, and protecting other types of tissues. It has a matrix, a substrate inside which the cellular component is found, which is, in turn, made up of specific cells (erythrocytes, leukocytes, -cysts). It is a renewable connective tissue.
The connective tissue develops from the embryonic mesenchyme tissue characterized by branched cells included in an abundant amorphous intercellular substance. Mesenchyme derives from the intermediate embryonic leaflet, mesoderm, very common in the fetus where it surrounds the developing organs by interpenetrating them. Some connective tissues of the skull derive directly from the neuroectoderm (meningeal fascia). The mesenchyme, in addition to producing all types of connective tissue, also makes other tissues: muscle, blood vessels, epithelium, and some glands.
The connective tissue is morphologically characterized by various types of cells (fibroblasts, macrophages, mast cells, plasma cells, leukocytes, undifferentiated cells, fat cells or adipocytes, chondrocytes, osteocytes, myofibroblasts, etc.). Immersed in an abundant intercellular material, called MEC (extracellular matrix). ECM (extracellular matrix). Synthesized from the same connective cells. Fundamental substance, erroneously defined amorphous, colloidal, formed by soluble complexes of carbohydrates, largely linked to proteins, called acid mucopolysaccharides, glycoproteins, proteoglycans, glucosaminoglycans or GAGs(hyaluronic acid, coindroitinsulfate, keratin sulfate, heparin sulfate, etc.) and, to a lesser extent, from specialized proteins, including fibronectin.
And
Cells and intercellular matrix characterize various types of connective tissue. Connective tissue proper ( connective tissue ), elastic tissue, reticular tissue, mucous tissue, endothelial tissue, adipose tissue, cartilage tissue, bone tissue, blood, and lymph. The connective tissues, therefore, play several vital roles. Structural, defensive, trophic, and morphogenetic by organizing and influencing the growth and differentiation of the surrounding tissues.
Protein fibers are, in fact, able to change according to the functional and ecological needs of their spectrum of structural and functional variability. The integument, the basement membrane, the cartilage, the bone, the ligaments, the tendons are examples, etc. The fundamental substance continuously changes its state. They are becoming more or less dense (from fluid to sticky to concrete), according to specific organic needs. Found in large quantities such as joint synovial fluid and ocular vitreous humor. It is present in all tissues.
The connective tissue varies its structural characteristics through the piezoelectric effect: any mechanical force that creates structural deformation stretches the inter-molecular bonds producing a slight electrical flow (piezoelectric charge).
And
The extracellular matrix provides the chemical-physical environment for the cells it envelops (thus taking part in the regulation of the acid-base balance, saline hydro metabolism, electrical and osmotic balance ), forming a structure to which they adhere and within which they can move maintaining a suitable hydrated and permeable ionic environment, through which they spread the metabolites. The density of the fibrous matrix and the viscosity of the fundamental substance determine the free flow of chemicals between cells while preventing the penetration of bacteria and inert particles. So, presents immune system cells (leukocytes, macrophages, mast cells, plasma cells) and is frequently the place where inflammatory processes take place. It also has excellent repairing capacity in areas damaged by inflammation and trauma, filling the spaces if necessary.
In the adipose tissue. Which constitutes a type of connective tissue. Lipids accumulate, significant nutritional reserves, while in the loose connective tissue, water and electrolytes are preserved (thanks to its high content of acid mucopolysaccharides). About 1/3 of the total plasma proteins are in the intercellular compartment of the connective tissue.
By combining a small variety of fibers within a matrix that varies from fluid to sticky to solid. The connective cells respond to the needs for flexibility and stability, diffusion, and barrier.
And
From a mechanical point of view. The tensions of movement and gravity while maintaining the shape of the different components of the body through the whole range of possibilities ranging from the rigidity of a continuous compression structure. To the elasticity of a tensegrity structure. In the tensegrity structure, the compression parts (the bones) push out against the traction parts (myofascial) that push inwards.
All the interconnected elements of a tensegrity structure rearrange themselves in response to local tension. The skeleton itself is only apparently a continuous compression structure. As the bones rest on slippery surfaces (articular cartilages) and without myofascial support, they are unable to sustain themselves. Therefore, varying the tension of the soft tissues means going the arrangement of the bones. Through the tensegrity network. All the remaining body parts.
The connective tissue and muscles constitute. Anatomically and functionally. The myofascial system, whose connective tissue is home to numerous sensory receptors. Including exteroceptors and nervous proprioceptors and structures. The muscles, anatomically and functionally, in myofascial chains. They are thus assuming a fundamental role in the internal balance and posture system.
And
So, It’s connective tissue network that we record posture and movement patterns through mechanical connective communication, which affects this more than the reflex mechanisms of the neuromuscular spindles and Golgi tendon organs(proprioceptive sense organs through which the nervous system inquiries about what happens in the myofascial network). It is, in fact, the myofascial system, the largest sensory organ of our organism. It is from it that the central nervous system receives mostly afferent (sensory) nerves. The presence of mechanoreceptors, in particular interstitial receptors, capable of causing effects at the local and general levels.
Connective tissue – myofascial systemin the myofascial (muscle-fascial) system of our body. Each muscle, visceral organ, vessel (blood and lymphatic), nerve, bone, joint, etc. These envelopes, in turn, form a ubiquitous network of tensegrity, which envelopes and, at the same time, supports and connects all the functional units of the body. Finally, these strong elastic layers also form a surface layer, which acts as a container and braking support for the whole body—the surface bands placed under the skin.
It is in the cell walls that divide it (epimysium, perimysium, and endomysium). Local “obstructions,” such as fascial adhesions, can result from excessive efforts or lack of exercise. Trauma, inflammatory diseases, adhesion scars, etc. In the presence of fascial adhesions in the different fascial layers. In particular, muscle stretching. This creates traction of the adjacent structures, which contributes to fatigue and general tensions.
And
Also, a muscle that works persistently in shortening. In addition to modifying the quality and quantity (based on the forces acting on it and the available spaces). The connective tissue portion can decrease. The number of sarcomeres (on the contrary, a muscle that works in lengthening tends to increase the connective part and the number of sarcomeres); this creates the formation of a retracted power. The elimination of these impediments and, therefore, the restoration of the correct flow allows the cells concerned to pass from a survival metabolism to a specific physiological one.
The discovery of the presence of connective tissue cells interposed with collagen fibers fascial is with contractile capacities similar to smooth muscles, called myofibroblasts, which has demonstrated the ability of the connective tissue to contract in certain situations.
How Vinyasa Yoga Benefits in Weight Loss
Regular dense connective tissue
Firstly, the dense (or compact) normal connective tissue can be found above Regular dense (or tight) connective tissue, all in the structures subjected to traction. In one direction (tendons, ligaments, aponeurosis, and fascia’s) and the stroma of the cornea. In other words, the tendons and ligaments. The fundamental amorphous substance is very scarce. The only cells present are fibroblasts arranged in long parallel rows in the interstices between the bundles of collagen fibers. In the fasciae and aponeuroses. The collagen fiber bundles have a less regular orientation than that of the tendons.
Finally, the connective tissue stroma of the cornea is characteristic. Approximately perpendicularly to those of the contiguous layer.
Connective tissue proper
- Lasso: The matrix (or fundamental substance) is very fragile and mainly consists of collagen (α-helix trimer).
- Elastin and in greater percentage fibrin (two proteins), which make it resistant and elastic. It is a support and connection structure between bone and musculature (e.g., Tendons).
- Elastic: In this case, elastin prevails in%, which therefore gives this fabric particular elastic properties. (eg. The ligaments).
Supportive connective tissue
- The matrix is semi-solid, very viscous, but still elastic. The main functions:
- filling;
- shock-absorbing pads: (joints; intervertebral discs);
- make certain parts of the body elastic (e.g., auricle, nose);
- support
- Osteoblasts and osteoclasts (cells capable of dissolving and reconstructing the bone matrix). The matrix contains oxen and is mineral (formed from calcium and magnesium phosphate). The histological structure of the bone tissue is the osteon formed by osteocytes and surrounded by concentric blades of the matrix.
Fluid connective tissue: characterized by a fluid matrix.
- Blood: (matrix: plasma) with the function of connecting all parts of the body. Formed by:
- Red blood cells (erythrocytes) have the function of transporting oxygen and are rich in hemoglobin.
- White blood cells (leukocytes) that take different names depending on the function they perform.
- Platelets (truncated cells) that thanks to thrombin (protein) allow blood clotting. (platelet cap).
- Adipose tissue: it has a reduced matrix as it is occupied by adipocytes. It has an insulating, shock-absorbing, and energy reserve function (triglycerides).
The technical advancement of electron microscopy has shown that the cell is far from a membranous sac containing a solution of molecules, as previously believed. So, the cell is actually full of filaments, tubes, fibers, and trabeculae, forming a structure called cytoplasmic matrix or cytoskeleton. There is very little space available to allow the random diffusion of molecules. Moreover, every little water is present in the free state is almost totally in the state of salvation as it happens for the connective tissue.
And
The cytoskeleton is mostly made up of actin microfilaments: a globular protein, and tubulin microtubules, a tubular protein. Microtubules and microfilaments are spontaneously formed and disintegrated when particular environmental conditions arise (e.g., presence of Ca2 + and Mg2 +).
In addition, already at the beginning of the eighties, the role of the cytoskeleton in support of the cell was understood in allowing the movements of the cell itself and of the vesicles and its implication in the processes of cell division. It is shown that the extracellular matrix is linked to the cytoskeleton system. So as to keep our body together. Today we know that these bonds affect physiological processes such as embryonic development, blood clotting, wound healing, etc.
What is DASH Diet and How the DASH Diet Can Help Your Cholesterol and Blood Pressure